Most dentists we talk to about dental revenue cycle management are working harder than ever, but their bank accounts don’t show it.They assume that if they produce the work, the money will eventually show up.
But here is the reality: the average dental practice is losing about 9% of its production revenue every single year simply because it isn’t being collected.
The Reality of Dental Revenue Cycle Management in 2026
Table of Contents
Most offices don’t realize what’s actually happening in their billing.
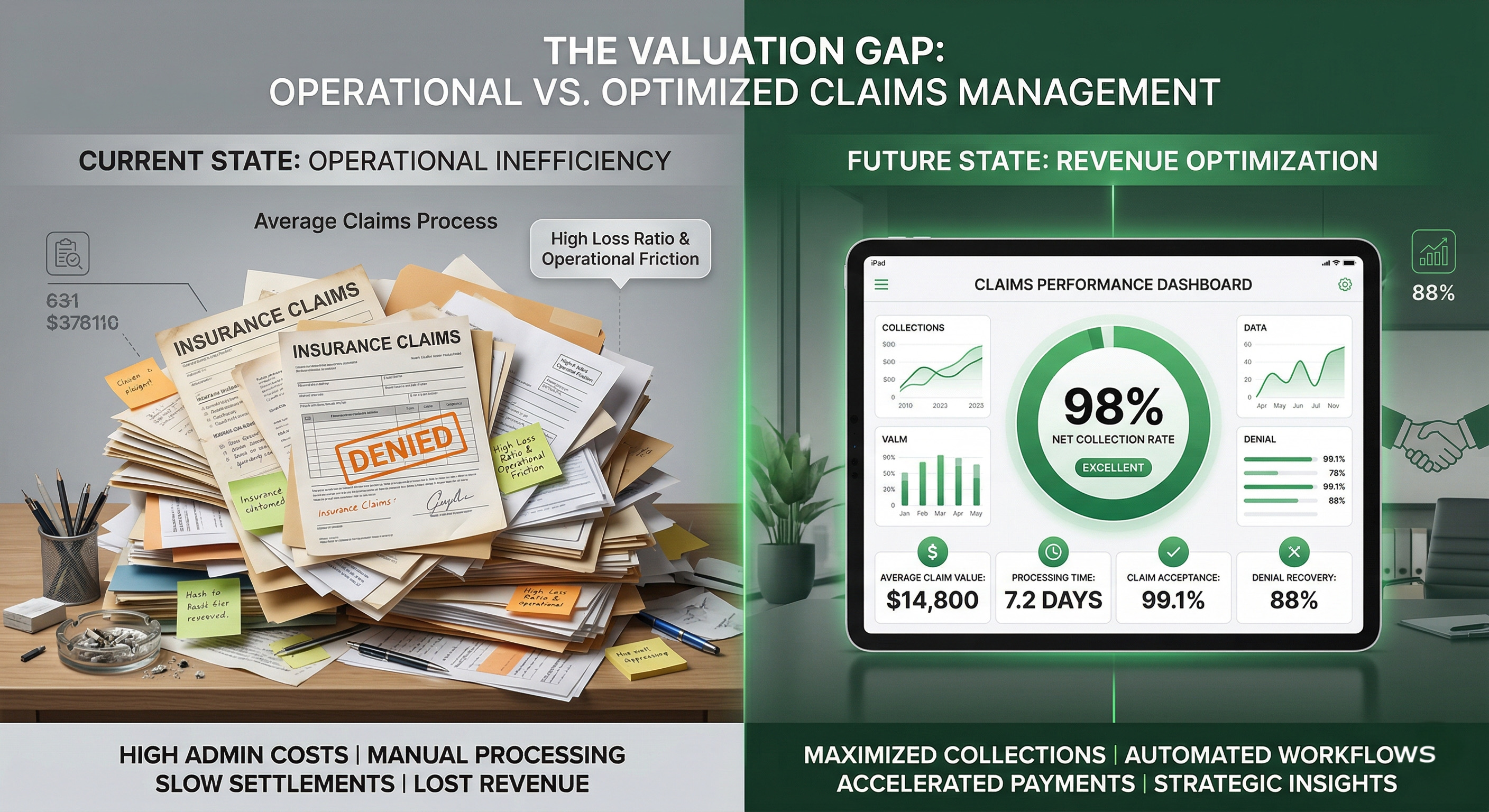
We see this more than we should. Offices celebrate a “98% collection rate,” but they are looking at the wrong number. They are looking at their Net collection rate after they’ve already written off thousands in PPO adjustments and “miscellaneous” errors.
The truth is that insurance companies are getting stricter. Recent data shows that 15% of all dental claims are denied on the first attempt. Even worse, about 77% of those denials have absolutely nothing to do with your clinical skill. They happen because of simple administrative blunders: a misspelled name, an outdated group ID, or a missing attachment.
The “Silent Killer” of your practice value.
This is a critical component of dental revenue cycle management that affects your practice’s exit strategy.
This is exactly why we tell our clients to stop looking at billing as just a front-desk task. It is a valuation task.
If you ever plan to sell your practice, a buyer is going to look at your aging reports. If they see a pile of money sitting in the “90+ days” bucket, they don’t see a future paycheck. They see a risk.
Look at how the age of your debt changes your chances of actually getting paid:
| Age of the Bill | Probability of Collection | The Financial Impact |
| 0–30 Days | 99% | Healthy cash flow |
| 31–60 Days | 70% | Delayed profit; needs monitoring |
| 61–90 Days | 30% | Problematic; money is “stuck” |
| 90+ Days | Less than 15% | High risk of total loss |
And this is a big one: in a formal practice sale, every dollar sitting in that 120-day bucket is often valued at zero. If you have $332,000 in uncollected debt and you are selling at a 6x multiple, that “small” billing problem just cost you $2 million in your sale price.
The 2026 Clean Claim Checklist
To avoid the 15% denial trap, your team should verify these three pillars before hitting “send”:
- Narrative Precision: Does the narrative explain why the treatment was necessary today? (e.g., “Recurrent decay under existing MO composite with fractured distal lingual cusp” vs. just “Broken tooth”).
- The 24-Hour Rule: Are claims being scrubbed and sent within 24 hours of the date of service? The fresher the data, the lower the error rate.
- Attachment Clarity: With carriers using AI to “read” X-rays, ensuring your images are high-contrast and clearly show the apex or interproximal decay is no longer optional—it’s a requirement for payment.
The PPO Fee Schedule Trap: Why “Standard” Isn’t Enough
Most practices treat their fee schedules as “set it and forget it” documents. However, in the world of dental revenue cycle management, an unoptimized fee schedule is a slow leak in your boat.
If you haven’t negotiated or updated your UCR (Usual, Customary, and Reasonable) fees in the last 18 months, you are likely leaving 5–12% of your potential revenue on the table. Carriers aren’t going to volunteer a raise; you have to prove the value of your chair time.
Three steps to reclaiming your margin:
- Benchmark Your Zip Code: Are your office fees in the 80th percentile for your area? If not, you’re capping your own reimbursement potential before the claim is even filed.
- Analyze the Write-Offs: If your write-offs for a specific carrier are exceeding 40%, it’s time to evaluate if that contract still serves your practice’s health.
- Coordination of Benefits (COB) Mastery: Secondary insurance is where most “hidden” money lives. If your team isn’t capturing the secondary fee schedule correctly, you’re essentially providing specialty care at a discount.
Why we do things differently at Steadfast.
Most billing companies, and even most in-house teams, work claims once a month. By the time they see a problem, the trail is cold.
Our approach to dental revenue cycle management involves weekly tracing. We don’t wait for a claim to hit 60 or 90 days before we start asking questions. We also know that a basic CDT code isn’t enough anymore. You need a narrative. You need a clinical story that tells the insurance reviewer why that crown was medically necessary and not just cosmetic.
When you provide the “Why” upfront, the insurance company has fewer excuses to hold your money.
If this sounds familiar, it might be time for a second set of eyes.
You didn’t go to school to become a professional debt collector. You went to school to be a doctor.
If you aren’t sure where your money is actually going, let’s dig into it. We offer a free billing analysis where we look at your real numbers, not the ones your software “cleans up” for you. We’ll show you exactly where the leaks are and how to plug them.
If you’re ready to professionalize your dental revenue cycle management, let’s talk.

Leave a Reply